HVAC and SARS-CoV-2 Manuscript Published in Indoor Air!
After publishing our preprint on SARS-CoV-2 and different locations within a hospital heating, ventilation, and air conditioning (HVAC) unit on MedRxiv, we submitted our article to Indoor Air. After five rounds of peer review, 4 reviewers, and nearly a year of revisions, it is now officially published! Check out the final version of the article here!

Over the course of May and June 2020, we sampled multiple of the AHUs at OHSU hospital. I’m gonna do my best as a biologist to describe the HVAC setup!
The GIANT air handling penthouse at the hospital is made up of 10 individual AHUs, each of which are more or less the same.

Air from the hospital returns, mixes with some portion of fresh outside air, is filtered through the pre-filters (MERV10), undergoes a second, more extensive filter (MERV15) at the final filters and then returns back to the hospital through the supply air dampers.
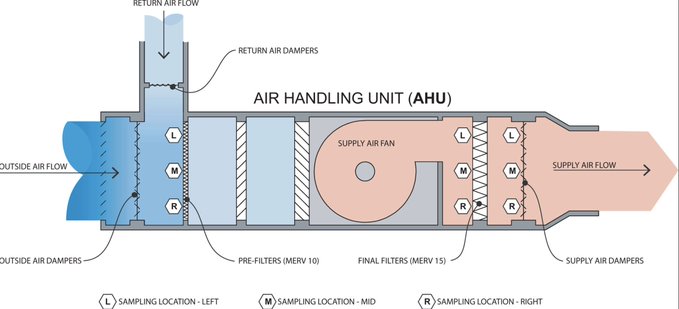
We took three samples at each of these three points (pre-filter, final filter, supply air damper) each time we were able to access the AHU. Samples were tested for the presence of SARS-CoV-2 RNA using qRT-PCR.

In short, we were able to detect the presence of SARS-CoV-2 RNA. We saw the highest abundance at the pre-filters and the second highest at the supply air dampers (!!). Yes, we saw significant abundance AFTER the MERV15 filters! Here are some important caveats to that data:
- We did not look at the potential viability of these samples, though it is unlikely, especially after filtering, that there were viable viral particles
- We have no evidence that these positives came from full genomes but could have instead been from genome fragments, again low likelihood of infectivity.
- At the point that we sampled, the filters had not recently been changed and the hospital had been admitting a large number of COVID+ individuals for months.
- On the other side of the coin, we suspect that swabbing these air filters is not the best way to do this sampling. Destructive sampling of the filters would have likely yielded higher abundances but was not possible for this study.
So, maybe filters aren’t perfect but we already knew this! No mitigation strategy is going to be 100%! The importance of these mitigation strategies is to layer them. So what can we do to layer on top of filters, especially outside of healthcare settings with MERV15 filters?
- Wear a mask! (Obvious caveats here)
- Increase ventilation and introduction of fresh air
- Maintaining relative humidity between 40-60%
- Use a HEPA air purifier in your home, office, etc…
- For your home AC/HVAC unit, use the highest rated filter your system can handle
Even more, we are moving into a new stage of the pandemic where detection in large areas is becoming more important. One of these such tools could be sampling of centralized HVAC systems in large buildings as individuals return back to work
How do you combat Covid-19 spreading through air conditioning?
— Bloomberg Quicktake (@Quicktake) August 10, 2020
Researchers at the University of Oregon say the key to safely reopening offices requires a better understanding of how pathogens move within a building #TheRebuild #COVID19 pic.twitter.com/BJPCcnbcmB
Built environment surveillance in general should be an integral and proactive component of a comprehensive infectious disease management strategy. By pairing these surveillance data with appropriate building operations layered risk reduction strategies, the transmission of disease indoors can be minimized and potentially avoided! Feel free to reach out through my email!
Abstract: Evidence continues to grow supporting the aerosol transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). To assess the potential role of heating, ventilation, and air conditioning (HVAC) systems in airborne viral transmission, this study sought to determine the viral presence, if any, on air handling units in a healthcare setting where coronavirus disease 2019 (COVID-19) patients were being treated. The presence of SARS-CoV-2 RNA was detected in approximately 25% of samples taken from ten different locations in multiple air handlers. While samples were not evaluated for viral infectivity, the presence of viral RNA in air handlers raises the possibility that viral particles can enter and travel within the air handling system of a hospital, from room return air through high-efficiency MERV-15 filters and into supply air ducts. Although no known transmission events were determined to be associated with these specimens, the findings suggest the potential for HVAC systems to facilitate transfer of virions to locations remote from areas where infected persons reside. These results are important within and outside of healthcare settings and may present necessary guidance for building operators of facilities that are not equipped with high-efficiency filtration. Furthermore, the identification of SARS-CoV-2 in HVAC components indicates the potential utility as an indoor environmental surveillance location.
